Blog
Choosing the right therapist: The 5 most important considerations
Choosing the right therapist can be difficult. Different problems and different personalities call for different therapies and different areas of expertise. What’s more, therapy is also both very personal — sometimes even confronting and upsetting — so you need someone you are very comfortable with.[...]
Creating Healthier Workspaces: How stress leave can foster happier, healthier, and more productive employees
Employee mental health is pivotal to overall workplace wellbeing, impacting individual performance, job satisfaction, and organisational productivity. The global pandemic certainly drew attention to employee mental health and shone a spotlight on just how important a healthy and supportive work environment is for fostering the best in employees. Employee mental health covers various factors, including [...]
From High Stakes to Healing: 8 Tips To Overcome Gambling Addiction
Gambling activities have become more accessible and convenient due to the proliferation of casinos and the rapid growth of online gambling platforms. Moreover, technological advancements and the rise of mobile devices have further integrated gambling into everyday life, creating additional risks for vulnerable individuals. Australian Gambling Statistics - Did you know? Some Facts According to the [...]
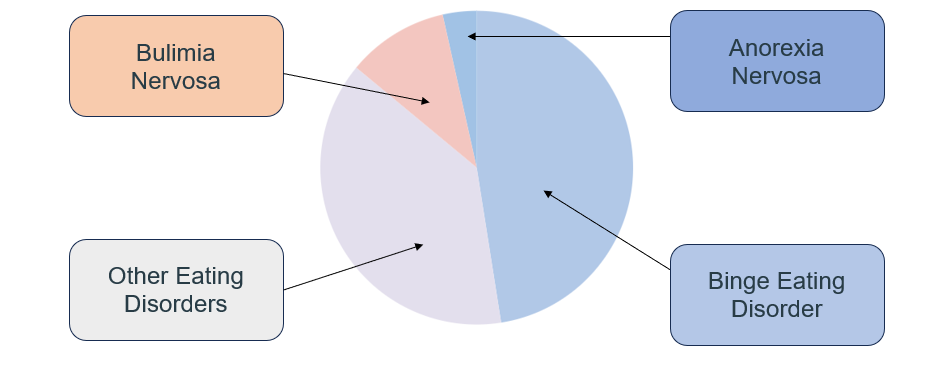
An Examination of Bulimia Nervosa Amongst Australian Celebrities
Bulimia nervosa is a serious eating disorder that can significantly impact an individual's physical and psychological health. Characterised by recurrent episodes of binge eating followed by compensatory behaviours, this condition can lead to severe health complications and emotional distress including low self-esteem, depression, and anxiety. Over time these behaviours can become more compulsive and uncontrollable. It is crucial to understand that individuals grappling with this disorder are not alone, and seeking professional assistance is par[...]
Tips on How to Stop Eating Junk Food
In today’s world, time efficiency and the desire for immediate satisfaction have become primary considerations for individuals. Junk food can provide this satisfaction because it not only tastes good, but it is convenient and easily accessible. Consequently, many people unconsciously engage in the consumption of unhealthy food in copious amounts. Consuming excess junk food can create a vicious cycle wherein the more one eats, the stronger and more consistent the cravings become. Although individuals possess cognitive knowledge regarding the [...]
Mental Health Statistics In Australia
According to the WHO, mental health is defined as a “state of well-being in which every individual realises his or her own potential, can cope with the normal stresses of life, can work productively and fruitfully, and is able to contribute to his/her community”. Mental health is a critical component of overall health and wellbeing, and it cannot be separated from other aspects of health. Mental health issues can have a flow-on effect, impacting the physical health and social relationships and vice-versa. If left untreated, mental health[...]
Therapist vs Psychologist? Understanding the basic differences between mental health professionals
Mental health has always been a critically important topic. But it’s only recently that a truly conscious effort has been made to openly discuss and raise awareness on the issue. Mental health is a pillar of overall wellbeing, and it cannot be separated from other aspects of health. Mental health issues can have a flow-on effect, impacting the physi[...]
Shocking Binge Drinking Facts For Australia – The Social Cost
At Bayside Psychotherapy in Melbourne, we’ve noticed an increase every year in the number of people we help to stop, or come to terms with the damaging impact of binge drinking. Whilst we help people from all walks of life, facing all kinds of personal challenges it’s clear that binge drinking and associated impacts of alcohol misuse are on the rise. Our counselling clinic is treating more people suffering with this out of control problem than we ever have before. View our presentation on Binge Drinking in Australia here: [U[...]